When Should I Get Another Covid Booster?
Here’s what you need to know about getting your next vaccine
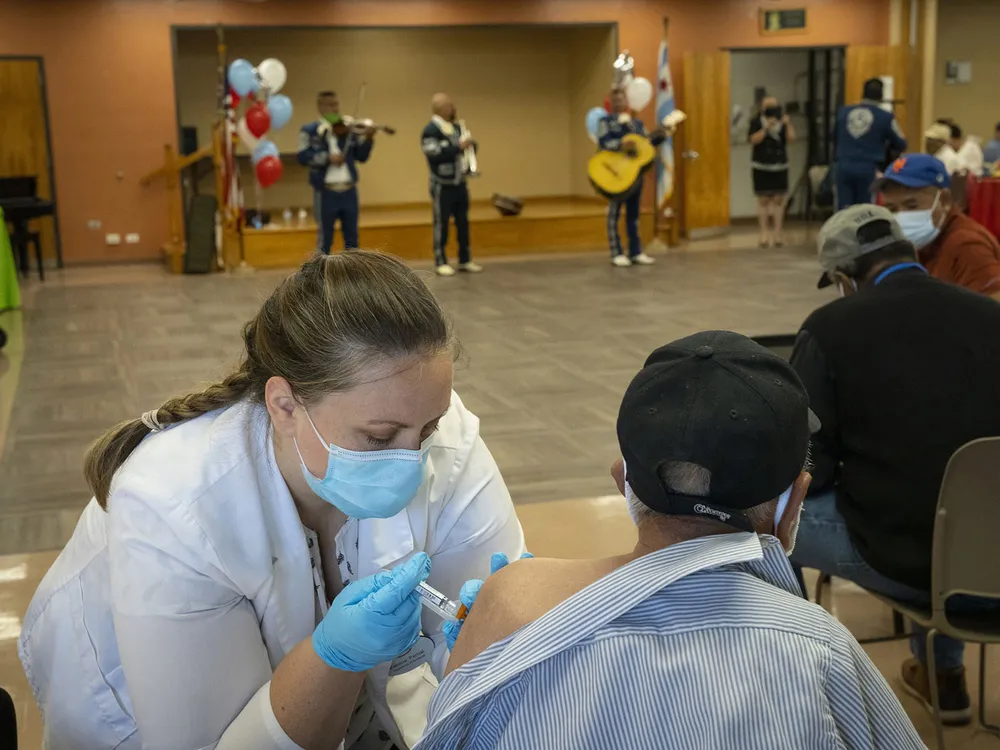
A trio of recent announcements have put Covid-19 vaccines and boosters back into the spotlight. On April 10, President Joe Biden signed a bipartisan resolution terminating the Covid-19 national emergency, which had allowed the government to free up funding and waive certain regulations to fight the pandemic. The same day, the White House announced the $5 billion Project Next Gen to develop the next generation of vaccines, as experts warned that current treatments were losing efficacy. And on April 19, the Centers for Disease Control and Prevention (CDC) allowed new boosters for older adults and immunocompromised patients.
Altogether, these updates paint a mixed portrait, recognizing the continued threat of Covid-19 to certain groups while also turning a page and looking toward the future. “We don’t want to let our guard down and normalize the situation,” says Ofer Levy, a pediatrician and director of the Precision Vaccines Program at Boston Children’s Hospital. “And on the other hand, we can’t be in an emergency footing forever. So how do we find that right balance?”
That has been the particular challenge over the past few years, with scientific breakthroughs accompanying unprecedented devastation. On one hand, the Covid-19 vaccine was developed in less than a year and has since fully inoculated over 230 million Americans, the fastest, most extensive vaccine rollout in history. On the other, over a million Americans died in what is now the deadliest pandemic ever for the United States, with the U.S. death toll surpassing that of any other country. Even as Covid-19 recedes from its position as America’s third-leading cause of death in 2022, it remains on track to be a top-ten cause of death this year with the emergence of new variants, such as XBB.1.5 (representing 84 percent of U.S. cases as of April 1).
Given the latest federal guidelines on boosters, the public understandably seeks clarity about what this all means for them. So, we’ve consulted medical experts to provide the answers.
Who should get a booster—and when?
Per the CDC, adults aged 65 or older can now receive another booster, provided they are at least four months removed from their last one. For individuals who are immunocompromised, they can now be boosted as frequently as every two months. Notably, all these boosters are bivalent, meaning that half of the shot protects against the original vaccine strain and the other half against the omicron strain.
Experts generally agree on this approach. As older adults have 5 to 15 times higher hospitalization rates and 60 to 360 times higher mortality rates than those ages 18 to 29, Levy notes that the most vulnerable groups should receive priority access to the second bivalent shot. For immunocompromised patients, “this small population does not build a strong enough immune response to the vaccines to begin with—which is why we’ve needed to boost them more,” says Brigham and Women’s Hospital emergency physician Jeremy Faust.
Ultimately, Levy suggests that people who feel they are at high risk should discuss with their doctors, making a joint decision about whether or not to get the booster—and when to get it. Booster efficacy wanes over time, with protection against severe infection resulting in hospitalization or death decreasing from 67 percent at week two to 38 percent at week 20, so the timing matters.
While older adults and immunocompromised individuals could get boosted right now, they could also get their doctor’s advice to time it better such that “if there’s a really big wave, high-risk people could come in and get another one whenever they want,” says Levy.
What should I do if I’m not older or immunocompromised?
For fully vaccinated younger adults, the question of whether to get a booster shot is less clear-cut. Levy again stresses the importance of remaining informed about the latest CDC recommendations and consulting with your doctor to make an informed risk assessment. In general, however, if a person has a healthy immune system, they can probably forgo the second bivalent booster because of substantial protection from the original series and such a low Covid-19 hospitalization rate among this group. For all demographics below 65 years old, the hospitalization rate is less than 2 per 100,000 people as of April 15.
Furthermore, when boosting outside the CDC guidelines, a real risk exists of imprinting, a suboptimal response where “your immune system remembers what it just saw and therefore, if it sees something different in the future, it may actually be less effective,” says Faust. In other words, constant boosters could overexpose a person’s immune system to specific viral features and thus make their system less responsive to strains without those features. Faust adds that older or immunocompromised individuals have the least risk of imprinting “because their immune memory isn’t that good.”
Although most Americans are not eligible for a second bivalent booster, the CDC emphatically recommends that adults of any age who are unvaccinated or just received the monovalent booster get a first bivalent booster. For people who are up to date on their Covid-19 vaccines but are still worried about the virus, Massachusetts General Hospital infectious disease physician Camille Kotton recommends they “ensure that everyone in their household is vaccinated,” especially when cohabitating with high-risk individuals. This strategy, called cocooning, protects immunocompromised individuals and older adults by forming “a layer of protection.”
How can we address booster hesitancy or lack of knowledge around updated recommendations?
While roughly 42 percent of U.S. adults aged 65 or over have received a bivalent booster, this proportion drops significantly for adults aged 18 to 65, to about 14 percent. But when it comes to vaccination promotion, Kotton points out a key distinction between these two groups. For young and middle-aged adults, the issue is often booster hesitancy; for older adults, it’s often a lack of information.
“The majority actually have not had a booster since September 2022,” says Kotton about the patients she sees in the hospital, “and actually tell me that they weren’t even aware that they needed to get a booster.” While the CDC’s booster-for-all message may have worked for some individuals last fall, its effectiveness waned in the long run, because resources were spread thin, according to Faust.
Given the very particular audience for this round of boosters, filling in knowledge gaps should be prioritized to ensure those at high risk can make a well-informed, balanced decision. Faust emphasizes that vaccinating vulnerable groups quickly is achievable; it’s merely “a logistical question. Do you know who they are and where they are? And are they willing? Are they interested?” Citing Israel’s success eradicating mpox via targeted vaccination of immunocompromised patients, Faust asserts that the CDC can accomplish more by focusing its outreach. For instance, the CDC could create partnerships with nursing homes and assisted living facilities to distribute information about the second bivalent booster, similar to past Covid-19 collaborations that provided staff with infection prevention training.
I heard the U.S. has ended the Covid-19 emergency designation. How does this affect booster access?
During the pandemic, most health insurance plans covered Covid-19 testing, treatments and vaccines without cost-sharing. With the emergency status lifted, those with insurance will likely continue to have vaccines covered, but out-of-pocket costs could accrue from at-home testing and treatment.
Meanwhile, people who are uninsured or underinsured—and on average faced significantly higher Covid-19 hospitalization and mortality rates—may have to start paying for vaccines, possibly forcing them to skip them. To address this concern, the Biden administration announced a $1.1 billion program to purchase vaccines for uninsured individuals. While certainly a welcome step, lack of knowledge about this initiative and its temporary nature raise questions as to whether access concerns will be fully resolved.
The emergency’s end will further compound this health insurance problem by eliminating the federal mandate for continuous Medicaid enrollment. In other words, an estimated 15 million people will be kicked off of Medicaid, with only a small percentage able to get coverage on the Affordable Care Act marketplace. While stopgap solutions can help ensure broad access to vaccines for the time being, without a more permanent solution, minority groups will be disproportionately impacted: In 2021, 18.8 percent of American Indian and Alaska Native populations and 17.7 percent of Hispanic communities were uninsured, compared to 5.7 percent of non-Hispanic whites. Thus, this vulnerable population that Faust says “deserves the most concern” may now face the largest barriers to getting the boosters.
Ultimately, what the end of the emergency signals is the political end to the pandemic, something wholly distinct from the pandemic’s medical and social end. “A lot of really creative ideas were inspired by the drastic situation we were under,” says Yale University public health biostatistician Jeffrey Townsend. “Without the emergency declaration, the medical establishment will be less able to move quickly.”
What does the future hold for Covid-19 vaccines?
Moving forward, the U.S. might consider pursuing a new yearly fall Covid-19 booster, with a supplementary spring option, according to Faust.
“There are a lot of lessons that can be learned from influenza vaccination, where the strains that are included in the annual influenza vaccination can change from year to year,” says University of Michigan decision scientist and health economist Lisa Prosser, “and that could potentially be the case here for a Covid booster as well.” Rather than continuing to use the current bivalent formulation, Covid-19 boosters could be adapted annually to target strains expected to dominate that season.
But setting such a regular booster schedule might not be sustainable, as “one of the big differences between Covid and the flu is that seasonality has not yet been clearly established,” according to epidemiologist Arnold Monto, also at the University of Michigan. With Covid-19 outbreaks in the summer and winter, timing boosters while being mindful of imprinting concerns becomes tricky. That’s why many public health professionals are excited about the Biden administration’s Project Next Gen, which will further investments in nasal and pan-coronavirus vaccines, with the goal of providing more durable protection against Covid-19 and future variants.
Some of these new technologies are already on the horizon, with at least four nasal vaccines in late-stage testing in people. Beyond being easier to administer, these vaccines can shut down the virus in the nose and throat, where all respiratory pathogens get their first foothold. Furthermore, the Duke Human Vaccine Institute recently created a pan-coronavirus vaccine that passed key laboratory and primate tests, as well as proved effective across many Covid-19 variants.
More broadly, experts hope that Project Next Gen will elicit sustained financial support for vaccinology, with advancements not just against Covid-19 but also against influenza, respiratory syncytial virus, HIV, Ebola and others. Such developments will require breaking the boom-and-bust cycle of investment, where “we throw huge amounts of money for a year or two, and then starve vaccinology as a field for 10 or 20 years until the next crisis,” Levy says.
The recent authorization of bivalent boosters is an important step for protecting our nation’s most vulnerable, but as new Covid-19 mutations continue to emerge, continued innovation offers the most promising substrate for truly bringing the pandemic to an end.